Hemorrhagic complications in COVID-19: three women with pectoral hematoma and a review
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Authors
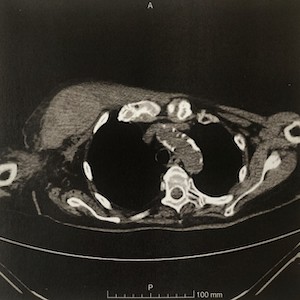
Patients hospitalized with COVID-19 pneumonia are at risk for thrombotic complications. At the same time, they need respiratory support, and they frequently require nursing in a prone position. From March to May 2020, 57 patients with acute respiratory distress syndrome were admitted to our departments. Our therapeutic protocol included anticoagulant treatment and prone positioning. We have treated three obese women affected by severe pneumonia and pectoral hematoma with post-hemorrhagic anemia. We have already described two of these cases in our previous publication; in this new article, we describe a third similar case and review clinical reports from 2020 to 2022 about hemorrhagic complications during COVID-19. Reports confirm that pectoral hematomas and bleeding in unusual sites are a complication of COVID-19. Pectoral hematomas are likely to be related to COVID-19 severity, heparin dosage, and traumatism due to cough and pronosupination.
Emergency department, MD
Emergency department, Director, MD
Internal Medicine department, Director, MD
How to Cite

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.






